Every day a provider sits credentialed but not yet cleared to see patients, a health system loses roughly $9,000 in revenue.
Ninety days of that? Over $800,000. Per provider.
And somehow, the companies selling the fix can’t explain why anyone should care.
That’s a healthcare marketing strategy problem. Not a product problem. Not a sales problem. The product works. The market is massive. But the way these companies talk about what they do is so generic, so interchangeable, so stuffed with “AI-powered” and “10x productivity” that buyers can’t tell one from the next.
This is the positioning gap that lives underneath every failing healthcare marketing strategy. And it costs more than most companies realize.
The $9,000 Math
Let’s make this concrete because the numbers matter.
The average physician generates $2.3 million annually. That’s roughly $9,200 per day. When credentialing takes 60 to 120 days (and it does, for most systems), that’s real revenue sitting on the table.
| Provider Specialty | Annual Revenue | Daily Revenue | 90-Day Delay Cost |
|---|---|---|---|
| Ophthalmology/Surgery | $2,600,000 | $10,400 | $936,000 |
| Average Physician | $2,300,000 | $9,200 | $828,000 |
| Dentist | $1,800,000 | $7,200 | $648,000 |
| Podiatrist | $1,500,000 | $6,000 | $540,000 |
Healthcare spent $20 billion on claim denials in 2022. More than 50% of those denials trace back to credentialing failures. Nearly 20% of organizations lose $500K or more annually because of credentialing errors alone.
This isn’t a back-office inconvenience. This is one of the most quantifiable revenue problems in healthcare.
So why does nobody talk about it that way?
When Every Healthcare Marketing Strategy Sounds the Same
I looked at four companies selling credentialing technology. Here’s what their marketing says:
- Company A: “AI-powered provider network infrastructure” with “intelligent automation”
- Company B: “AI-powered platform” that “streamlines network management”
- Company C: “Automated data collection” that “speeds onboarding”
- Company D: “First autonomous agent built to unlock 10x team productivity”
Close your eyes. Shuffle them. Can you tell which is which?
Neither can buyers.
This is what a broken healthcare marketing strategy looks like from the outside. Four companies, four versions of the same sentence, four interchangeable value propositions. And when buyers can’t tell the difference, they default to three things: price, incumbent relationship, or whatever their consultant recommends.
That’s not a market. That’s a coin flip.
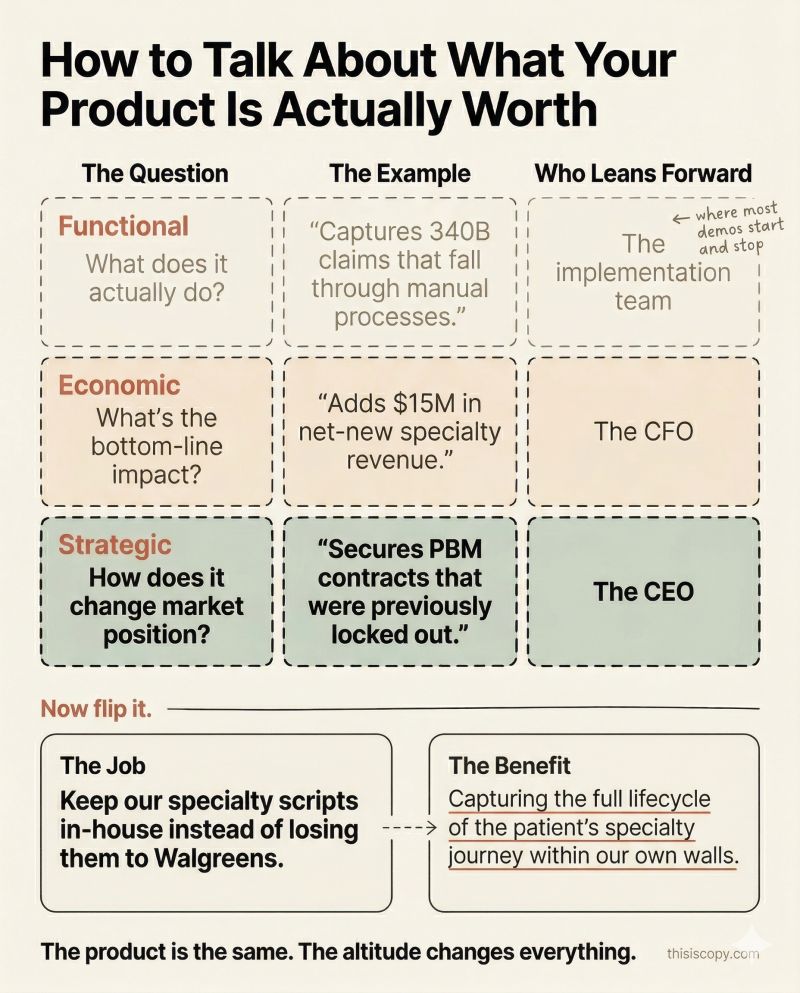
The Revenue Frame That Nobody Uses
Here’s what’s wild. I listened to podcast interviews with leadership at one of these companies. And the way they talk about the product privately is completely different from how they market it publicly.
In interviews, the leadership frames credentialing as revenue infrastructure. They describe provider data as “grease or rust” on operational levers. They talk about the strategic advantage of bringing credentialing in-house instead of outsourcing it.
On the website? “AI-powered automation.” “10x productivity.” “Audit-ready accuracy.”
It’s a Severance problem. The outie (leadership on podcasts) knows exactly what the product means. The innie (the marketing site) has no memory of that conversation at all. Two versions of the same company, walled off from each other.
| What Leadership Says (Interviews) | What the Website Says |
|---|---|
| “Credentialing as a revenue lever” | “10x team productivity” |
| “Eliminating the hidden bottleneck” | “AI-powered automation” |
| “Revenue acceleration infrastructure” | “Audit-ready accuracy” |
| “Strategic competitive advantage” | “Autonomous agents” |
The word “revenue” is completely absent from the primary marketing. Despite leadership using it in every conversation.
This is the gap. The healthcare marketing strategy fails not because the team doesn’t understand the product. It fails because the positioning work hasn’t been done to bridge what leadership knows and what the website communicates.
The 12% Problem
A January 2026 industry report found something that should terrify every healthcare marketing strategist:
Only 12% of organizational AI investments touch credentialing and enrollment.
The overwhelming majority goes to clinical and patient-facing use cases. But the same organizations reporting this allocation also report losing over $1 million annually to credentialing bottlenecks.
They know the problem exists. They know it costs real money. But they’re not investing in fixing it.
Three reasons:
Executive advocacy gap. Credentialing departments don’t have the organizational voice that clinical leaders do. There’s no Chief Credentialing Officer. Nobody’s championing this at the board level.
Time horizon bias. Clinical AI gets positioned as long-term strategic transformation. Administrative AI gets categorized as “immediate but minor.” So it never makes the priority list. (This is the Interstellar problem. One hour on the clinical AI planet equals seven years of credentialing delays back on Earth. The time cost is real, you just can’t see it from where you’re standing.)
Problem perception. Credentialing delays are treated as an unavoidable business tax. Something you endure, not something you solve. And when a problem feels inevitable, nobody goes looking for a solution.
A good healthcare marketing strategy doesn’t just describe the product. It reframes the problem. It makes the buyer see something they’ve been tolerating as something they should be fixing.
Five Segments, Five Different Conversations
Here’s where healthcare marketing strategy gets specific. Because “healthcare” isn’t one buyer. And credentialing isn’t one problem.
There are at least five distinct buyer segments, each feeling the pain differently:
1. The Outsourcing Escape (~800 organizations)
These systems outsourced credentialing to a CVO and regret it. Turnaround exceeds 45 days. Quality control is a mess. They have zero real-time visibility into their own credentialing pipeline.
The marketing message isn’t “our AI is better.” It’s “you can bring this back in-house without doubling your headcount.” One payer brought credentialing in-house and saved seven figures while cutting turnaround from 45 to 60 days down to less than a week.
2. The Network Expansion Bottleneck (~1,200 organizations)
These are systems doing M&A, launching new sites, or expanding telehealth. Every one of them has a 90-day credentialing backlog throttling their growth ROI.
They don’t need “automation.” They need the 90-day backlog turned into a 2-week sprint. That’s a completely different conversation than “10x productivity.”
3. The Burnout Spiral (~2,000 organizations)
Staff turnover above 30%. Unfilled vacancies. Teams stretched so thin that one resignation creates a cascade. The 38% admin burnout rate in healthcare isn’t a stat to these teams. It’s Tuesday.
The marketing message here is operational survival. Not efficiency.
4. The Compliance Fire (~600 organizations)
NCQA audit findings. CMS penalties. 25 to 50% denial rates. Civil penalties that make the CFO’s eye twitch.
For these buyers, “audit-ready” isn’t a feature. It’s the reason they’re on your website in the first place.
5. The Network Adequacy Squeeze (~500 organizations)
CMS is tightening network adequacy enforcement in 2026. Plans that can’t demonstrate adequate provider networks face enrollment restrictions and financial penalties.
Network adequacy is a credentialing speed problem. The marketing strategy should say exactly that.
The Hierarchy Problem
Most healthcare marketing strategies are built feature-first. The hierarchy looks like:
- Mechanism: Here’s what our technology does
- Outcome: Here’s the result you’ll get
That’s backwards. The buyer doesn’t care about the mechanism until they believe the outcome is worth pursuing. I broke down exactly how this shelf problem works in my analysis of Regard’s positioning statement.
A better hierarchy (and a better healthcare marketing strategy):
- Context shift: Credentialing is a revenue accelerator, not a compliance cost. The $9,000-per-day problem is the most quantifiable revenue leakage in healthcare.
- Category claim: The outsourced CVO model is obsolete. Strategic insourcing is a competitive advantage.
- Proof: Here’s the case study. Here are the numbers. Here’s how it works.
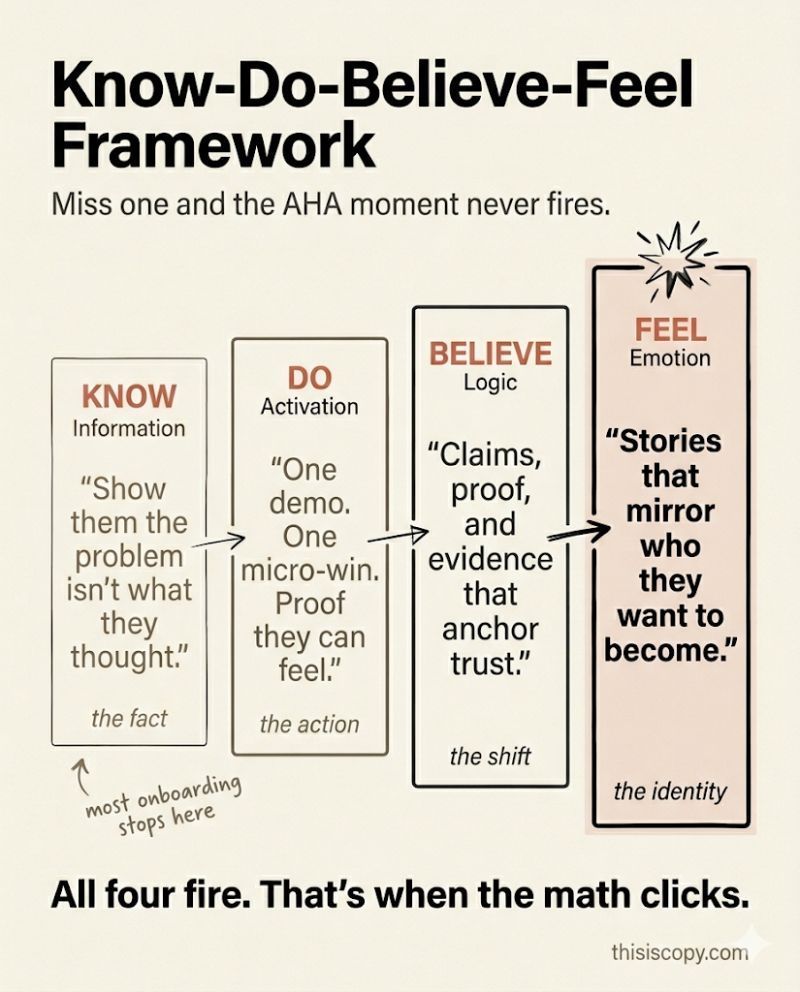
The mechanism comes last. Because nobody cares how you do it until they believe the problem is worth solving.
That’s the work of positioning. Reframing what buyers believe before showing them what you sell.
What This Means for Your Healthcare Marketing Strategy
If you’re running marketing for a B2B healthcare company and your messaging sounds interchangeable with three competitors, you don’t have a messaging problem. You have a positioning problem wearing a messaging costume.
The fix isn’t better copywriting (although that helps). The fix is going upstream:
- Listen to how your leadership talks about the product in interviews. That’s usually closer to the truth than your website.
- Listen to how buyers describe you in case studies. If their language doesn’t match your homepage, your positioning is lagging behind your product.
- Segment your buyers by pain, not by firmographics. Five different problems need five different conversations.
- Lead with the context shift, not the mechanism. Make the buyer believe the problem is worth solving before you show them how you solve it.
The $9,000-per-day gap isn’t just a credentialing problem. It’s a healthcare marketing strategy problem. And the company that frames it best will own the category.
See how positioning becomes messaging in practice. 150 real before and after examples from B2B healthcare companies.